If you're a Dentist looking to discuss one of our services,
40 Years Of Wisdom,
Choose The Best.
Work with us
DENTISTS: LOOKING TO DISCUSS OUR SERVICES?
40 Years of Wisdom.
Choose The Best
Work With Us
PROVIDING DENTISTS WITH EXCEPTIONAL RESULTS
Vancouver’s Premium
Dental Laboratory
For over 45 years, Ocean Ceramics has been providing high-quality dental prosthetics to our clients around Vancouver, BC. Our company has grown because of our strong team and our ability to keep up with dentistry’s ever-changing technology. The creation of our sister entities, Denta4 and Trio Creations, has allowed us to become the full-service dental laboratory that we are today. Learn more about Ocean Ceramic’s company history, our team and what our clients have to say about our work.

Book a free 15 minute consultation!
Interested in our dental laboratory services? We would be happy to discuss how our services can benefit you and your dental practice. Schedule a free 15 minute online consultation today!
Full-Service Dental Laboratory in
British Columbia
Ocean Ceramics is a full-service dental laboratory located in Coquitlam, BC that provides dental prosthetics for dentists and their clients. Our dental laboratory services include crown and bridge restorations, implants, dentures, hybrids, sleep appliances, dental materials, continuing education and more!
Crown & Bridge
We offer a wide variety of dental crown & bridge prosthetic services. Learn more about our dental crowns & bridges we offer and our processing times.
Removables
Our removables include dentures, sleep appliances, snore guards and more! Learn more about our removable and our 1-2-3 removables technique.
Implants
We have in-depth knowledge of implants and offer a wide variety of dental implant prosthetics. Learn more about dental implants at our dental
laboratory.
Hybrids
We offer hybrid bridges which combine the use of gingival tissue and teeth together in one bridge. Learn more about our zirconia and acrylic hybrid bridges.
RX Slipss
We require various pieces of information to help us provide high-quality dental prosthetics. View our RX Slips and resources here!
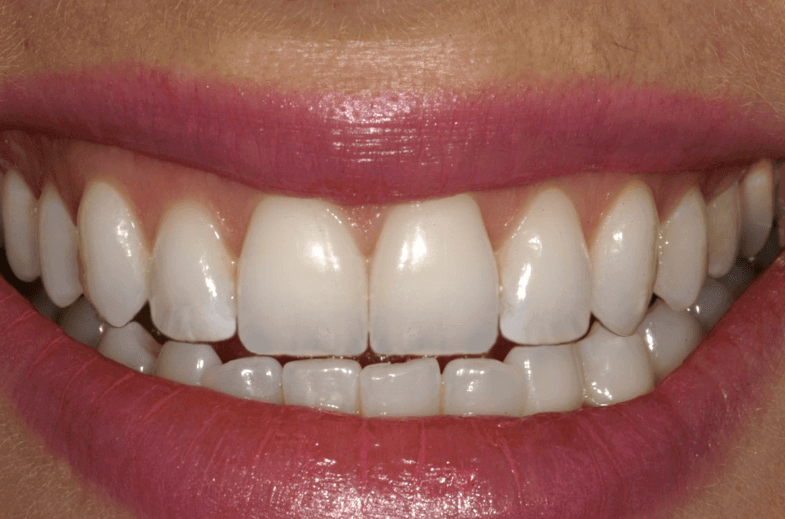
MySmile™ Designs at Ocean Ceramics
MySmile™ designs were created to give dentists and patients the ability to see an initial vision of what their new smile might look like. MySmile™ designs are used to create a treatment plan to achieve the desired smile aesthetics as closely as possible. Depending on the clinical situation involving the hard or soft tissues, the end results may vary. Learn more about how Ocean Ceramics uses MySmile™ designs.
Ocean Ceramic’s Photo Protocol
Ocean Ceramics uses dental photo records when making custom dental prosthetics for clients. These records are provided to allow us to assess the patient’s smile and help us gain a better understanding of how their smile is going to be improved. Our dental technicians use them as a useful visual tool when creating dental prosthetics. We have specific photo protocols at Ocean Ceramics that will help us ensure a high-quality design. Learn more about how to use Ocean Ceramic’s photo protocols with your patients.


Denta4’s Certified Training & Educational Course
Denta4 is a sister entity to Ocean Ceramics that offers dental professionals training and education courses related to diagnosing, treating, and restoring compromised airways and jaw joints. This training allows you to provide your patients with optimal and accurate solutions so that you’re not restoring your patient’s teeth to poor occlusions. Completing our Denta4 training and education courses will give you the confidence to successfully complete cases with our team supporting you along the way.
Client Testimonials
We take pride in our work with Dentists across Vancouver and surrounding areas. Check
out what our clients have to say about working with our team at Ocean Ceramics.
ABOUT US
Ocean Ceramics is a
dental lab in Vancouver,
BC that educates and delivers full and partial mouth reconstruction, including implants, crowns and prosthetics.
CONTACT US
Ocean Ceramics Ltd.
#1-3180 262nd Street
Aldergrove, BC
V4W 2Z6
1(604) - 777 - 1337
OUR FAMILY
Ocean Ceramics
Denta4
Trio

